SPINAL DYSRRAPHYSM
The human nervous system develops from a small, specialized plate of cells along the back of an embryo. Early in development, the edges of this plate being to curl up toward each other, creating the neural tube –a narrow sheath that closes to form the brain and spinal cord of the embryo. As development progresses, the top of the tube becomes the brain and the remainder becomes the spinal cord. The process is usually complete by the 28th day of pregnancy. But if problems occur during this process, the result can be brain disorders, called neural tube defects, including spina bifida.
WHAT IS SPINA BIFIDA?
Spina bifida, which literally means “split spine”, is characterized by the incomplete development of the brain, spinal cord, and/or meninges (the protective covering around the brain and spinal cord). It is the most common neural tube defect.
WHAT ARE THE DIFFERENT TYPES OF SPINA BIFIDA?
There are four types of spina bifida: occulta, closed neural tube defects, meningocele, and myelomeningocele.
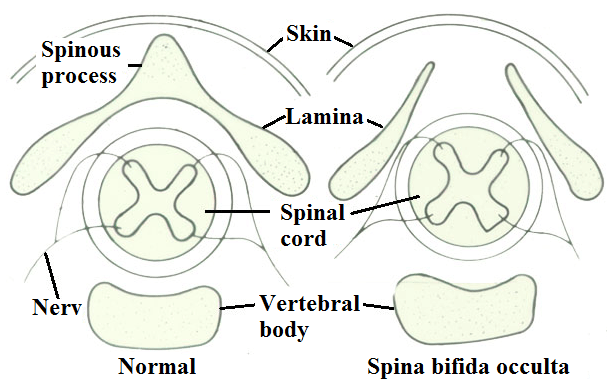 |
Occulta is the mildest and most common form in which one or more vertebrae are malformed. The name “occulta”, which means “hidden”, indicates that the malformation, or opening in the spine, is covered by a layer of skin. This form of spina bifida rarely causes disability or symptoms.
|
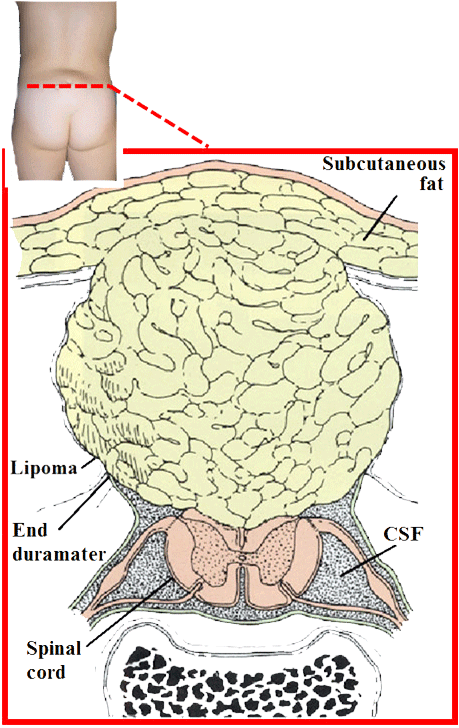
Closed neural tube defects make up the second type of spina bifida. This form consists of a diverse group of spinal defects in which the spinal cord is marked by a malformation of fat (lipomyelomeningocele), bone (diastematomyelia), or membranes. In some patients there are few or no symptoms; in others the malformation causes incomplete paralysis with urinary and bowel dysfunction.
 |
 |
|
Axial cut in lipomyelomeningocele
|
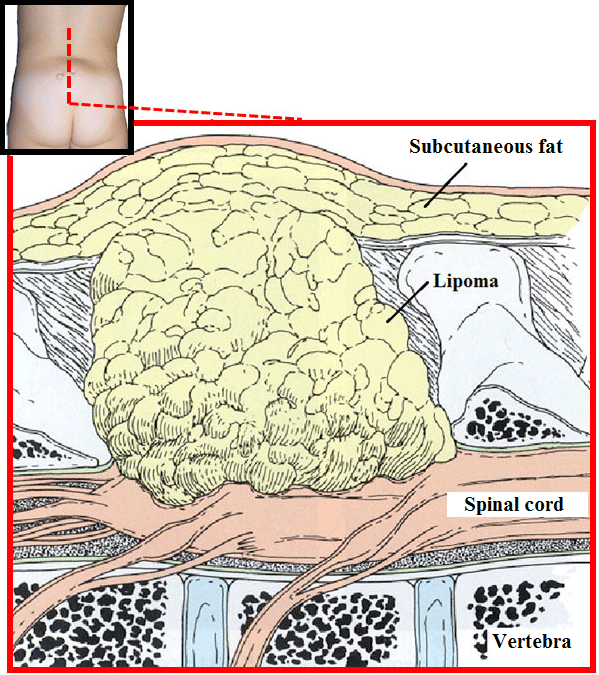
Sagittal cut in lipomyelomeningocele
|
 |
|
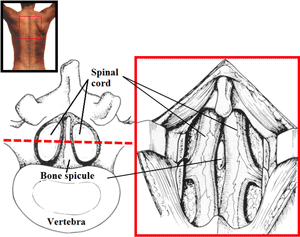
Diastematomyelia: on the left coronal outline and on the right of the surgical field exposure after removal of muscle mass, spinous processes and laminae
|
In the third type, meningocele, the meninges protrude from the spinal opening, and the malformation may or may not be covered by a layer of skin. Some patients with meningocele may have few or no symptoms while others may experience symptoms similar to closed neural tube defects.
 |
Myelomeningocele, the fourth form, is the most severe and occurs when the spinal cord is exposed through the opening in the spine, resulting in partial or complete paralysis of the parts of the body below the spinal opening. The paralysis may be so severe that the affected individual is unable to walk and may have urinary and bowel dysfunction.
|
|
Myelomeningocele
|
 |
 |
|
Sagital section in myelomeningocele
|
Axial section in myelomeningocele
|
What causes spina bifida?
The exact cause of spina bifida remains a mystery. No one knows what disrupts complete closure of the neural tube, causing a malformation to develop. Scientist suspect genetic, nutritional, and environmental factors play a role. Research studies indicate that insufficient intake of folic acid –a vitamin- in the mother’s diet is a key factor in causing spina bifida and other neural tube defects. Prenatal vitamins that are prescribed for the pregnant mother typically contain folic acid as well as other vitamins.
What are the signs and symptoms of spina bifida?
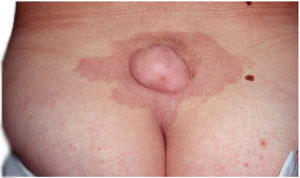
The symptoms of spina bifida vary from person to person, depending on the type. Often, individuals with occulta have no outward signs of the disorder. Closed neural tube defects are often recognized early in life due to an abnormal tuft or clump of hair or a small dimple or birthmark on the skin at the site of the spinal malformation.
 |
 |
 |
|
Dimple in the skin marking the existence of a dermal sinus
|
Anomalous hair marking diastematomyelia
|
Skin angioma and lumbosacral lipoma
|
Meningocele and myelomeningocele generally involve a fluid-filled sac-visible on the back- protruding from the spinal cord. In meningocele, the sac may be covered by a thin layer of skin, whereas in most cases of myelomeningocele, there is no layer of skin covering the sac and a section of spinal cord tissue usually is exposed.
What are the complications of spina bifida?
Complications of spina bifida can range from minor physical problems to severe physical and mental disabilities. It is important to note, however, that most people with spina bifida are of normal intelligence. Severity is determined by the size and location of the malformation, whether or not skin covers it, whether or not spinal nerves protrude from it, and which spinal nerves are involved. Generally all nerved located below the malformation are affected. Therefore, the higher the malformation occurs on the back, the greater the amount of nerve damage and loss of muscle function and sensation.
In addition to loss of sensation and paralysis, another neurological complication associated with spina bifida is Chiari II malformation –a rare condition (but common in children with myelomeningocele) in which the brainstem and the cerebellum, or rear portion of the brain, protrude downward into the spinal canal or neck area. This condition can lead to compression of the spinal cord and cause a variety of symptoms including choking, arm stiffness, and difficulties with feeding, swallowing, and breathing.
Chiari II malformation may also result in a blockage of cerebrospinal fluid, causing a condition called hydrocephalus, which is an abnormal build-up of cerebrospinal fluid in the brain. Cerebrospinal fluid is a clear fluid that surrounds the brain and spinal cord. The build-up of fluid puts damaging pressure on the brain. Hydrocephalus is commonly treated surgically implanting a shunt –a hollow tube- in the brain to drain the excess of fluid into the abdomen.
Some newborns with myelomeningocele may develop meningitis, an infection in the meninges. Meningitis may cause brain injury and can be life-threatening.
Children with both myelomeningocele and hydrocephalus may have learning disabilities, including difficulty paying attention, problems with language and reading comprehension, and trouble learning math.
Additional problems such as latex allergies, skin problems, gastrointestinal conditions, and depression may occur as children with spina bifida get older.
How is it diagnosed?
In most cases, spina bifida is diagnosed prenatally (before birth). However, some mild cases may go unnoticed until after birth, or posnatally. Very mild cases, in which there are no symptoms, may never be detected.
Prenatal diagnosis
The most common screening method used to look for spina bifida during pregnancy are second trimester maternal serum alpha fetoprotein (MSAFP) screening and foetal ultrasound. The MSAFP screen measures the level of a protein called alpha-fetoprotein (AFP), which is made naturally by the foetus and placenta. During pregnancy, a small amount of AFP normally crosses the placenta and enters the mother’s bloodstream. But if abnormally high levels of this protein appear in the mother’s bloodstream it may indicate that the foetus has a neural tube defect. The MSAFP test, however, is not specific for spina bifida, and the test cannot definitively determine that there is a problem with the foetus. If a high level of AFP is detected, the doctor might request additional testing, such as an ultrasound or amniocentesis to help determine the cause.
The second trimester MSAFP screen described above may be performed alone or as part of a larger, multiple-marker screen. Multiple-marker screens look not only for neural tube defects, but also for other birth defects, including Down syndrome and other chromosomal abnormalities. First trimester screens for chromosomal abnormalities also exist but signs of spina bifida are not evident until the second trimester when the MSAFP screening is performed.
Amniocentesis –an exam in which the doctor removes samples of fluid from the amniotic sac that surrounds the foetus- may also be used to diagnose spina bifida. Although amniocentesis cannot reveal the severity of spina bifida, finding high levels of AFP may indicate that the disorder is present.
Postnatal diagnosis
Mild cases of spina bifida not diagnosed during prenatal testing may be detected post-natally by X-ray tests performed during a routine examination. Doctors may use magnetic resonance imaging (MRI) or a computed tomography (CT) scan to get a clearer view of the spine and vertebrae. Individuals with the more severe forms of spina bifida often have muscle weakness in their feet, hips, and legs. If hydrocephalus is suspected, the doctor may request a CT scan and/or X-ray of the skull to look for extra fluid inside the brain.
How is the spina bifida treated?
There is no cure for spina bifida. The nerve tissue that is damaged or lost cannot be repaired or replaced, nor can function be restored to the damaged nerves. Treatment depends on the type and severity of the disorder. Generally, children with the mild form need no treatment, although some may require surgery as they grow.
The key priorities for treating myelomeningocele are to prevent infection from developing through the exposed nerves and structures from additional trauma. Typically, a child born with spina bifida will have surgery to close the defect and prevent infection or further trauma within the first few days of life.
 |
|
Steps in the surgical repair of a myelomeningocele
|
Doctors have recently begun performing foetal surgery for treatment of myelomeningocele. Foetal surgery –which is performed in uterus (within uterus) – involves opening the mother’s abdomen and uterus and sewing shut the opening over the developing baby’s spinal cord. Some doctors believe the earlier the defect is corrected, the better the outcome is for the baby. Although the procedure cannot restore but lost neurological function, it may prevent additional loss from occurring. However, the surgery is considered experimental and there are risks to the foetus as well as to the mother.
The major risks to the foetus are those that might occur if the surgery stimulates premature delivery such as organ immaturity, brain haemorrhage, and death. Risks to the mother include infection, blood loss leading to the need for transfusion, gestational diabetes, and weight gain due to bed rest.
Still, the benefits of foetal surgery are promising, and include less exposure of the vulnerable spinal nerve tissue and bone to the intrauterine environment, in particular to the amniotic fluid, which is considered toxic. As an added benefit, doctors have discovered that the procedure affects the way the brain develops in the uterus, allowing certain complications –such as Chiari II Malformation with associated hydrocephalus– to correct them selves, thus, reducing or, in some cases, eliminating the need for surgery to implant a shunt.
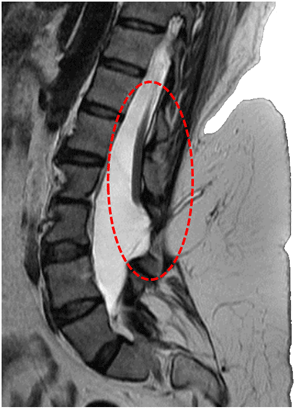
Many children with myelomeningocele develop a condition called progressive tethering, or tethered cord syndrome, in which their spinal cords become fastened to an immovable structure –such as overlying membranes and vertebrae- causing the spinal cord to become abnormally stretched and the vertebrae elongated with growth and movement. This condition can cause loss of muscle function to the legs, bowel, and bladder. Early surgery on the spinal cord may allow the child to regain a normal level of functioning and prevent further neurological deterioration.
 |
 |
 |
|
Sagittal MRI in tethered spinal cord due to untreated in myelomeningocele
|
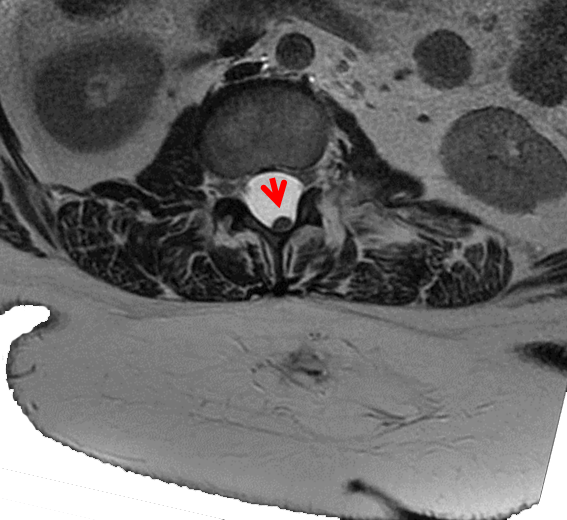
Coronal MRI in tethered spinal cord due to untreated in myelomeningocele
|
Coronal MRI in tethered spinal cord due to untreated in myelomeningocele
|
Some children will need subsequent surgeries to manage problems with the feet, hips, or spine. Individuals with hydrocephalus generally will require additional surgeries to replace the shunt, which can be outgrown or become clogged.
Some individuals with spina bifida require assistive devices such as braces, crutches, or wheelchairs. The location of the malformation on the spine often indicates the type of assistive devices needed. Children with a defect high on the spine and more extensive paralysis will often require a wheelchair, while those with a defect lower on the spine may be able to use crutches, bladder catheterizations, leg braces, or walkers.
Treatment for paralysis and bladder and bowel problems typically begins soon after birth, and may include special exercises for the legs and feet to help prepare the child for walking with braces or crutches when he or she is older.
Can the disorder be prevented?
Folic acid, also called folate, is an important vitamin in the development of a healthy foetus. Although taking this vitamin cannot guarantee having a healthy baby, it can help. Recent studies have shown that by adding folic acid to their diets, women of childbearing age significantly reduce the risk of having a child with a neural tube defect, such as spina bifida. Therefore, it is recommended that all women of childbearing age consume 400 micrograms of folic acid daily. Foods high in folic acid include dark green vegetables, egg yolks, and some fruits. Many foods –such as some breakfast cereals, enriched breads, flours, pastas, rice, and other grain products- are now fortified with folic acid. Many multivitamins contain the recommended dosage of folic acid as well.
Women who have a child with spina bifida, have spina bifida themselves, or have already had a pregnancy affected by any neural tube defect are at greater risk of having a child with spina bifida or another neural tube defect. These women may require more folic acid before they become pregnant.