LOW BACK PAIN
WHAT IS ACUTE LOW BACK PAIN?
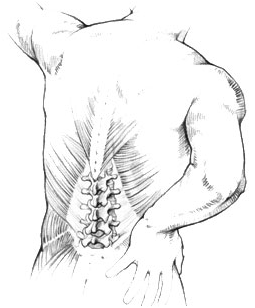 |
Acute low back pain (LBP) is defined as low back pain which persists for at least 6 weeks. It may be experienced as aching, burning, stabbing or dull pain, and might be felt as well-defined or vague. Its intensity may range from mild to severe and fluctuate over time (days). Acute LBP itself may spread into one or both buttocks, into the thigh/hip area, or even further down reaching the feet. LBP may begin following a strenuous activity or a jarring trauma, but its onset can also be spontaneous and unrelated to a specific physical activity. The pain may begin suddenly or develop gradually. At least 80% of individuals experience a significant episode of LBP at some point in their lives. |
WHAT CAUSES ACUTE LBP?
 |
The exact cause of acute LBP is often difficult to identify. Acute LBP sources can be muscles, fascia of the connective tissue, ligaments, joint capsules, cartilage, and even blood vessels in the area. These tissues may be pulled, strained, stretched or sprained, leading to LBP. In addition, annular tears (small tears that occur in the outer layer of the intervertebral disc) can also initiate LBP, which in these cases is usually severe. When a tissue is irritated, no matter which type of tissue it is, a cascade of events involving anti-inflammatory agents, which cause pain, unfolds. These agents are released in response to tissue irritation and stimulate the surrounding pain-sensitive nerve fibers, resulting in more pain. Some of these substances trigger inflammatory responses (swelling), which also contribute to the pain and may persist for days or even weeks. Muscular tension may induce a spasm, resulting in a «trunk shift» (the body tilts to one side more than the other) due to muscular imbalance. |
HOW LONG WILL THE PAIN LAST?
 |
Usually, even if the exact cause of pain is not determined, the pain subsides spontaneously over time. 50% of episodes are resolved within 2 weeks, and 80% by 6 weeks. Unfortunately, however, the duration and severity of a single episode cannot be predicted based on the onset, location of pain, or even on the initial severity. Excruciating initial pain may resolve within a few days, while moderate or mild symptoms may persist for weeks. However, up to 30% of individuals will experience recurrent pain or develop persistent pain in the future. The symptoms of acute LBP are usually benign and self-limited. Even a ruptured disc has a chance of improving without surgery. On rare cases, however, LBP is caused by a more serious process such as a fracture, an infection, or cancer. This is more common in individuals over 50 years old, in those with a history of cancer, those with severe LBP at rest, and in those with associated fever or underlying medical problems, such as diabetes, heavy alcohol or drug use, long time corticosteroid use, and osteoporosis. |
|
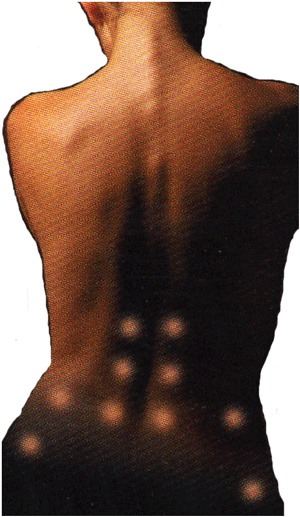
Distribution areas of LBP
|
Pain or weakness in the legs, or difficulty with bowel or bladder control, justify prompt medical consultation. If the pain lasts longer than 6 weeks, medical evaluation is strongly recommended.
WHAT IS THE TREATMENT FOR LBP?
Active rest, i.e. reducing physical activity but trying not to completely eliminate it, is recommended. Physical activity keeps blood and nutrients flowing to the affected area, reducing the inflammation and muscular tension. Many people who suffer from LBP find that they can perform their usual activities (e.g. walking), just in a more controlled way, and that, despite the pain, they feel better after the activity. More vigorous activities that require higher intensity, such as weight lifting, sports competitions, or contact sports, are inadvisable while the pain is severe.
There is no reason to avoid stretching leg and back muscles or tissues during an episode of acute LBP, but stretching should not aggravate the pain.
Local application of heat or ice can temporarily reduce pain, and heat may facilitate stretching, but will not necessarily speed long term recovery.
Non-steroidal anti-inflammatory drugs (NSAIDs) are analgesic (relieve pain) and anti-inflammatory. They can reduce the intensity of acute LBP, but their use can be accompanied by side effects, especially if taken for prolonged periods. The most common side effects are erosive gastritis with stomach ulcer, haemorrhages, osteoporosis, and liver and kidney problems.
Muscle relaxants reduce the muscle spasms, and, with it, pain is reduced too. They act on the central nervous system, producing drowsiness and reducing emotional tension. It should be noted, though, that they can make driving more difficult.
Opioids are very powerful analgesics with a sedating effect, so can be useful to facilitate sleep. However, their long-term use is associated with unpleasant side effects, including physical dependence, sedation, depression, constipation, and itching.
Other treatments, such as physiotherapy, ultrasound, transcutaneous electric neuro-stimulation (TENS), traction, passive mobilisation and chiropractic manipulation can provide temporary relief, but may not improve long-term recovery. It is usually useful, however, to ask the physiotherapist for specific strategies to recover motility and safely resume daily activities.
In the majority of cases, acute LBP is resolved spontaneously. For those in which LBP persist or recurs, medical assessment and an exercise program scheduled by a physiotherapist are recommended. The goal will be to achieve an independent lifestyle or a regular exercise schedule, and emphasis will be put in optimising core strength and improving general flexibility as well as cardiovascular endurance.
Spinal injections are usually not considered an appropriate treatment for acute, self-limited LBP. There are various injection options for persistent or recurrent pain, including steroid administration in the facet joint, epidural space, or at the point where the pain is originated.
DO I NEED AN X-RAY OR AN MRI?
Diagnostic tests are recommended when there is a history of severe trauma, cancer, fever, diabetes, drug abuse, bowel or bladder dysfunction, nocturnal pain, osteoporosis, or if the patient is over 50 years old. When the pain is severe, sometimes these tests will be recommended to investigate its cause.
There are several imaging techniques, amongst which we find regular X-ray, CT scan, MRI, and bone density scan. The choice of test will depend on the symptoms and on what medical condition is suspected. The final diagnosis, however, will depend on the clinical history, physical examination and complementary diagnostic test results.
Acute LBP can be a very painful experience, but fortunately it is often resolved quickly. When the pain does not improve satisfactorily, a series of tests must be started to investigate the cause of the pain and determine the most suitable treatment. The main objective is to resolve the acute episode as quickly as possible and to prevent future episodes through appropriate education, exercise and fitness.