MINIMALLY INVASIVE SPINAL SURGERY IN GENERAL
WHAT MAKES MINIMALLY INVASIVE SPINAL SURGERY DIFFERENT?
Conventional spinal surgery requires large incisions in the back. Muscles are cut and completely separated (temporarily) from the spinal column to allow access to the area. This produces large scars and, above all, leaves large muscle areas devascularised and denervated, causing atrophy in those muscles, which after the surgery will no longer work as before. Usually, blood loss is great and the surgical intervention is long. Due to all this, conventional spinal surgery cannot be applied to people with compromised general condition, advanced age or presence of other co-existing diseases (diabetes, hypertension, heart or lung disease, obesity…).
On the other hand, minimally invasive spinal surgery is performed through small incisions in the back. This leads to small scars and minimal damage to the muscle mass, so the recovery is fast and the risk of sequelae is significantly smaller than in conventional open spinal surgery. However, complex equipment is required and the surgeon must have had highly specialised training, so these techniques are not available in all hospitals or for all surgeons.
We thus conclude that, although both types of surgery seek to correct the problems of the spinal column and the nervous tissue that it contains, minimally invasive spinal surgery minimises the damage to surrounding tissues, especially the muscles.
WHAT ARE THE RISKS AND BENEFITS OF MINIMALLY INVASIVE SPINAL SURGERY?
Minimally invasive surgery is often used for many surgical interventions, such as gall bladder removal or bariatric surgery (surgery for obesity). It has recently been applied to procedures on the spine, including spinal decompression and spinal fusion.
Minimally invasive surgery has many advantages over conventional spinal surgery:
- Smaller incisions (so less pain and better aesthetic result)
- Less blood loss
- Shorter hospital stay (so costs are reduced)
- Less analgesics
- Work and daily activities resumed in a shorter amount of time
 |
 |
|
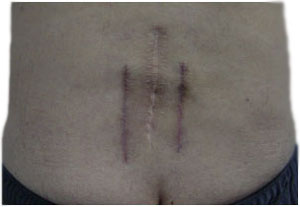
Skin incisions after open field lumbar postero-lateral arthrodesis
|
Skin incisions after percutaneous lumbar postero-lateral arthrodesis
|
 |
 |
|
Skin incisions after open field sacroiliac joint arthrodesis
|
Skin incisions after percutaneous sacroiliac joint arthrodesis
|